Glenohumeral Arthritis
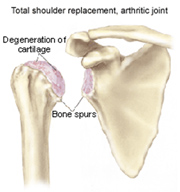
What is glenohumeral arthritis?
The glenohumeral joint is the shoulder joint, and arthritis is the loss of articular cartilage. There are varying stages of this condition, with different treatments depending on the severity of the arthritis.
What treatments are given?
As with all shoulder conditions, we first offer a course of non-operative care. Depending what treatments have been previously given, this may include non-steroidal anti-inflammatory medications, relative rest from the activities that aggravate the condition, and other activity modification. We will obtain plain X-rays of the shoulder, to aid in the diagnosis of glenohumeral arthritis, and to evaluate the severity of the arthritis.
One of the treatment modalities we recommend is physical therapy. In the case of arthritis, the goal of therapy is to maintain the shoulder motion a patient already has, and to help strengthen the shoulder musculature, including the rotator cuff, that may be deconditioned from decreased use due to pain. The most successful portion of therapy is a home program that patients are taught, and when done on a regular basis, can be quite helpful in achieving the treatment goals.
Another treatment we offer is a cortisone injection. Cortisone is an injectable anti-inflammatory medication, which is often very effective in helping with pain relief. In glenohumeral arthritis, we inject the cortisone directly into the shoulder joint, where the medication can help decrease the inflammation, and thus decrease the pain, associated with the arthritis. Any more than three injections may actually cause the rotator cuff tendon to weaken, and may cause some further problem with the cartilage.
Finally, if nonsurgical treatments fail, or become less effective over time, we may offer surgical treatment. Surgery is reserved for patients who are experiencing pain on a regular, if not constant basis, who have limited ability to use the shoulder, due to pain or loss of motion, and whose quality of life has decreased to the point where they would consider surgical intervention.
What are the surgical treatment options?
The basis for surgical treatment of arthritis is to remove the arthritis, and replace it with biologic, metal and/or plastic parts to help regain function of the joint. Hip and knee replacements are quite common, and shoulder replacement is becoming more common. In the past, shoulder replacement surgery has been more difficult, with less predictable results, but over the last two decades, technology and technique of shoulder surgery have significantly improved, and now we can offer shoulder replacement surgery with more reliable outcomes.
Each patient who elects to undergo shoulder replacement is evaluated on the basis of the arthritis and the rotator cuff. When the patient's arthritis is severe, throughout the entire joint, a total shoulder replacement is the best treatment option, if that patient has a functioning rotator cuff. We remove the arthritic humeral head, and replace it with a metal ball. The ball is attached to a stem that is put down inside the humerus for stability. The glenoid (cup) is also prepared. Here, the arthritis is also removed, and the glenoid is resurfaced with a plastic cup.
If the patient has severe arthritis, but has a large, non-repairable rotator cuff tear, the best treatment option may be a reverse total shoulder replacement.
In some patients, the arthritis is localized to one side of the joint, either the humeral head (ball) or the glenoid (cup) side. In these cases, the surgery may be less involved, but still involves removing the arthritis and resurfacing the joint.
In isolated humeral head arthritis, we approach the joint in the same way, and will often do a hemiarthroplasty, or partial shoulder replacement. This can involve placing a similar ball and stem as the total shoulder, or in young patients, with stronger bone, it may involve placing a "hemi-cap," which is a metal cap shaped like the humeral head, over the arthritic area.
What is the post-operative protocol?
Post-operatively, patients are placed into a sling and advised to do only gentle pendulum exercises. Each patient is admitted to the hospital overnight, and will stay from one to two days. No active motion is allowed, to protect the repaired subscapularis tendon, allowing this to heal. Patients return to the office between 10 and 14 days for a wound check, suture removal, and at that time, physical therapy is prescribed. For the first six weeks patients focus on passive and active assisted motion, and at six to eight weeks after surgery, active motion is started with some gentle strengthening. If all goes as anticipated, the total recovery time is approximately four months. Unfortunately, some patients have some postoperative stiffness, or even other problems, which may increase the time of recovery.
Xrays are taken at the first postoperative visit, as a baseline, and again at three and six months after surgery followed by yearly on the anniversary of the surgery. These xrays are taken yearly to ensure that the shoulder replacement remains in good position, without failure. If there is evidence of early failure, the xrays will help us see this, and any repeat surgery that may be necessary is less complex and has a better recovery time.
We have found that most patients (90%-95%) are very satisfied with their results in regards to pain relief and improved function. Most of the remaining patients (who are less satisfied), still have an improved result, but are not fully satisfied because they may have some residual pain or decreased motion.
Our goal at Middlesex Orthopedic Surgeons is to provide high quality care, both non-surgical and surgical, that will allow patients to experience pain relief and regain lost function resulting in the improvement of their quality of life. Through state of the art care, our ultimate aim is to facilitate our patients' return to a satisfactory level of function.
Are You Considering Shoulder Replacement Surgery?
Circumstances vary, but generally patients are considered for total joint replacement if:
- Functional limitations restrict not only work and recreation, but also the ordinary activities of daily living
- Pain is not relieved by more conservative methods of treatment – such as medications (including, for the shoulder, injections of cortisone, a powerful anti-inflammatory medication) and physical therapy – and/or by restricting activities
- Stiffness in the joint is marked and, in the shoulder, significantly limits range of motion of the arm
- X-rays show advanced arthritis or other problems
Ready to Consider Shoulder Joint Replacement?
Some Things You Should Know Replacement of an arthritic or injured shoulder is less common than knee or hip replacement. When necessary, however, shoulder replacement typically provides the same potential benefits as those procedures, including relief of joint pain and restoration of more normal joint movement.
Restoration of movement is particularly important in the shoulder, the body mechanism that allows your arm to rotate in every direction. If you're experiencing severe shoulder pain and reduced shoulder movement, there are probably many daily activities you can no longer do – or do as well or as comfortably – as before your shoulder problems began.
There are two types of shoulder joint replacement procedures:
- A Partial Shoulder Joint Replacement is used when the glenoid socket is intact and does not need to be replaced. In this procedure, the humeral component is implanted, and the humeral head is replaced.
- A Total Shoulder Joint Replacement is used when the glenoid socket needs to be replaced. All three shoulder joint components are used in this procedure.
How Long Will an Artificial Shoulder Joint Last? How long a joint replacement will last is impossible to predict. Individual results vary. As successful as most of these procedures are, over the years the artificial joints can become loose and unstable or wear out, requiring a revision (repeat) surgery. Many factors determine the outcome including:
- Age
- Activity level
- Bone strength
- Bone quality
- Disease progression
Loosening is a common cause of joint replacement surgery failure. A small amount of loosening and bone loss will occur. If it reaches a certain degree, a revision surgery may be indicated.
Possible Complications of Surgery
As with any major surgical procedure, patients who undergo total joint replacement are at risk for certain complications; however, the vast majority can be successfully avoided and/or treated. In fact, the complication rate following joint replacement surgery is very low: serious complications, such as joint infection, occur in less than 2% of patients.
Besides infection, possible complications include blood clots (the most common complication) and lung congestion, or pneumonia. Some shoulder-specific complications that may occur are nerve injury – since many major nerves and blood vessels travel through the armpit (axilla) – and dislocation, particularly just after the replacement surgery.
Complications may require medical intervention including additional surgery and, in rare instances, may lead to death. Your doctor should discuss these potential complications with you.
After the Surgery
During your hospital stay, your orthopaedic specialist works closely with nurses, physical therapists, and other healthcare professionals to ensure the success of your surgery and rehabilitation. Usually a case manager is assigned to work with you as you move through your rehabilitation routines. As the days progress, expect to become more independent in your movements.
If you need to work with a physical therapist after your joint replacement, the therapist will begin an exercise program to be performed in bed and in the therapy department. The physical therapist will work with you to help you regain muscle strength and increase range of motion.
When fully recovered, most patients with shoulder replacements can return to work and normal daily activities. However, individual results vary. If you are considering doing any of the following activities – which could potentially affect how long your artificial shoulder will last and how well it will perform – discuss it first with your doctor or orthopaedic specialist:
Any activity that places excessive stress on your shoulder joint such as: Lifting or pushing heavy objects, Hammering and other forceful arm/shoulder movements, Boxing and other arm/shoulder impact sports.
The success of your joint replacement will strongly depend on how well you follow your orthopaedic specialist's instructions. As time passes, you have the potential to experience a dramatic reduction in joint pain and a significant improvement in your ability to participate in daily activities.
Dr. David Hergan is a shoulder arthritis surgeon specializing in the treatment of glenohumeral arthritis in the Connecticut area. For all appointments and inquiries, please call (860) 669-4197 (860) 669-4197 or click here to request an online appointment.





